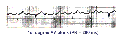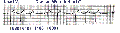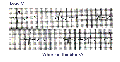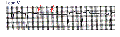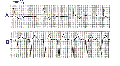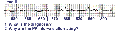6. ECG Conduction Abnormalities
Topics for Study:
Introduction:
This section considers all the important disorders of impulse conduction that may occur within the cardiac conduction system illustrated in the above diagram. Heart block can occur anywhere in the specialized conduction system beginning with the sino-atrial connections, the AV junction, the bundle branches and their fascicles, and ending in the distal ventricular Purkinje fibers. Disorders of conduction may manifest as slowed conduction (1st degree), intermittent conduction failure (2nd degree), or complete conduction failure (3rd degree). In addition, 2nd degree heart block occurs in two varieties: Type I (Wenckebach) and Type II (Mobitz). In Type I block there is decremental conduction which means that conduction velocity progressively slows down until failure of conduction occurs. Type II block is all or none. The term exit block is used to identify conduction delay or failure immediately distal to a pacemaker site. Sino-atrial (SA) block is an exit block. This section considers conduction disorders in the anatomical sequence that defines the cardiac conduction system; so lets begin . . .
Sino-Atrial Exit Block (SA Block):
2nd Degree SA Block: this is the only degree of SA block that can be recognized on the surface ECG (i.e., intermittent conduction failure between the sinus node and the right atrium). There are two types, although because of sinus arrhythmia they may be hard to differentiate. Furthermore, the differentiation is electrocardiographically interesting but not clinically important.
Type I (SA Wenckebach)
The following 3 rules represent the classic rules of Wenckebach, which were originally described for Type I AV block. The rules are the result of decremental conduction where the increment in conduction delay for each subsequent impulse gets smaller until conduction failure finally occurs. This declining increment results in the following findings:
- PP intervals gradually shorten until a pause occurs (i.e., the blocked sinus impulse fails to reach the atria)
- The pause duration is less than the two preceding PP intervals
- The PP interval following the pause is greater than the PP interval just before the pause
Differential Diagnosis: sinus arrhythmia without SA block. The following rhythm strip illustrates SA Wenckebach with a ladder diagram to show the progressive conduction delay between SA node and the atria. Note the similarity of this rhythm to marked sinus arrhythmia. (Remember, we cannot see SA events on the ECG, only the atrial response or P waves.)
Type II SA Block
- PP intervals fairly constant (unless sinus arrhythmia present) until conduction failure occurs.
- The pause is approximately twice the basic PP interval
Atrio-Ventricular (AV) Block
Possible sites of AV block:
- AV node (most common)
- His bundle (uncommon)
- Bundle branch and fascicular divisions (in presence of already existing complete bundle branch block)
1st Degree AV Block
PR interval > 0.20 sec; all P waves conduct to the ventricles.
2nd Degree AV Block
The diagram below illustrates the difference between Type I (or Wenckebach) and Type II AV block.
In "classic" Type I (Wenckebach) AV block the PR interval gets longer (by shorter increments) until a nonconducted P wave occurs. The RR interval of the pause is less than the two preceding RR intervals, and the RR interval after the pause is greater than the RR interval before the pause. These are the classic rules of Wenckebach (atypical forms can occur). In Type II (Mobitz) AV block the PR intervals are constant until a nonconducted P wave occurs. There must be two consecutive constant PR intervals to diagnose Type II AV block (i.e., if there is 2:1 AV block we can't be sure if its type I or II). The RR interval of the pause is equal to the two preceding RR intervals.
- Type I (Wenckebach) AV block (note the RR intervals in ms duration):
Type I AV block is almost always located in the AV node, which means that the QRS duration is usually narrow, unless there is preexisting bundle branch disease.
- Type II (Mobitz) AV block(note there are two consecutive constant PR intervals before the blocked P wave):
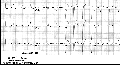
- Type II AV block is almost always located in the bundle branches, which means that the QRS duration is wide indicating complete block of one bundle; the nonconducted P wave is blocked in the other bundle. In Type II block several consecutive P waves may be blocked as illustrated below:
Complete (3rd Degree) AV Block
- Usually see complete AV dissociation because the atria and ventricles are each controlled by separate pacemakers.
- Narrow QRS rhythm suggests a junctional escape focus for the ventricles with block above the pacemaker focus, usually in the AV node.
- Wide QRS rhythm suggests a ventricular escape focus (i.e., idioventricular rhythm). This is seen in ECG 'A' below; ECG 'B' shows the treatment for 3rd degree AV block; i.e., a ventricular pacemaker. The location of the block may be in the AV junction or bilaterally in the bundle branches.
AV Dissociation (independent rhythms in atria and ventricles)
- Not synonymous with 3rd degree AV block, although AV block is one of the causes.
- May be complete or incomplete. In complete AV dissociation the atria and ventricles are always independent of each other. In incomplete AV dissociation there is either intermittent atrial capture from the ventricular focus or ventricular capture from the atrial focus.
- There are three categories of AV dissociation (categories 1 & 2 are always incomplete AV dissociation):
Intraventricular Blocks
Right Bundle Branch Block (RBBB)
- "Complete" RBBB has a QRS duration ≥ 0.12s
- Close examination of QRS complex in various leads reveals that the terminal forces (i.e., 2nd half of QRS) are oriented rightward and anteriorly because the right ventricle is depolarized after the left ventricle. This means the following:
- Terminal R' wave in lead V1 (usually see rSR' complex) indicating late anterior forces
- Terminal S waves in leads I, aVL, V6 indicating late rightward forces
- Terminal R wave in lead aVR indicating late rightward forces
- The frontal plane QRS axis in RBBB should be in the normal range (i.e., -30 to +90 degrees). If left axis deviation is present, think about left anterior fascicular block, and if right axis deviation is present, think about left posterior fascicular block in addition to the RBBB.
- "Incomplete" RBBB has a QRS duration of 0.10 - 0.12s with the same terminal QRS features. This is often a normal variant.
- The "normal" ST-T waves in RBBB should be oriented opposite to the direction of the terminal QRS forces; i.e., in leads with terminal R or R' forces the ST-T should be negative or downwards; in leads with terminal S forces the ST-T should be positive or upwards. If the ST-T waves are in the same direction as the terminal QRS forces, they should be labeled primary ST-T wave abnormalities
Left Bundle Branch Block (LBBB)
- "Complete" LBBB" has a QRS duration ≥ 0.12s
- Close examination of QRS complex in various leads reveals that the terminal forces (i.e., 2nd half of QRS) are oriented leftward and posteriorly because the left ventricle is depolarized after the right ventricle.
- The "normal" ST-T waves in LBBB should be oriented opposite to the direction of the terminal QRS forces; i.e., in leads with terminal R or R' forces the ST-T should be downwards; in leads with terminal S forces the ST-T should be upwards. If the ST-T waves are in the same direction as the terminal QRS forces, they should be labeled primary ST-T wave abnormalities. In the above ECG the ST-T waves are "normal" for LBBB; i.e., they are secondary to the change in the ventricular depolarization sequence.
- "Incomplete" LBBB looks like LBBB but QRS duration = 0.10 to 0.12s, with less ST-T change. This is often a progression of LVH.
Left Anterior Fascicular Block (LAFB)... the most common intraventricular conduction defect
- Left axis deviation in frontal plane, usually -45 to -90 degrees
- rS complexes in leads II, III, aVF
- Small q-wave in leads I and/or aVL
- R-peak time in lead aVL > 0.04s, often with slurred R wave downstroke
- QRS duration usually < 0.12s unless coexisting RBBB
- Usually see poor R progression in leads V1-V3 and deeper S waves in leads V5 and V6
- May mimic LVH voltage in lead aVL, and mask LVH voltage in leads V5 and V6.
Left Posterior Fascicular Block (LPFB).... Very rare intraventricular defect!
- Right axis deviation in the frontal plane (usually > +100 degrees)
- rS complex in lead I
- qR complexes in leads II, III, aVF, with R in lead III > R in lead II
- QRS duration usually < 0.12s unless coexisting RBBB
- Must first exclude (on clinical grounds) other causes of right axis deviation such as cor pulmonale, pulmonary heart disease, pulmonary hypertension, etc., because these conditions can result in the identical ECG picture!
Bifascicular Blocks
- RBBB plus either LAFB (common) or LPFB (uncommon)
- Features of RBBB plus frontal plane features of the fascicular block (axis deviation, etc.)
Nonspecific Intraventricular Conduction Defects (IVCD)
- QRS duration > 0.10s indicating slowed conduction in the ventricles
- Criteria for specific bundle branch or fascicular blocks not met
- Causes of nonspecific IVCD's include:
- Ventricular hypertrophy (especially LVH)
- Myocardial infarction (so called periinfarction blocks)
- Drugs, especially class IA and IC antiarrhythmics (e.g., quinidine, flecainide)
- Hyperkalemia
Wolff-Parkinson-White Preexcitation
Although not a true IVCD, this condition causes widening of QRS complex and, therefore, deserves to be considered here
QRS complex represents a fusion between two ventricular activation fronts:
- Early ventricular activation in region of the accessory AV pathway (Bundle of Kent)
- Ventricular activation through the normal AV junction, bundle branch system
ECG criteria include all of the following:
- Short PR interval (< 0.12s)
- Initial slurring of QRS complex (delta wave) representing early ventricular activation through normal ventricular muscle in region of the accessory pathway
- Prolonged QRS duration (usually > 0.10s)
- Secondary ST-T changes due to the altered ventricular activation sequence
QRS morphology, including polarity of delta wave depends on the particular location of the accessory pathway as well as on the relative proportion of the QRS complex that is due to early ventricular activation (i.e., degree of fusion).
Delta waves, if negative in polarity, may mimic infarct Q waves and result in false positive diagnosis of myocardial infarction.